I am a PhD student and a practicing extended scope physiotherapist and I’d like to find out how my NHS colleagues can use information from quality improvement projects to change care for the better. If your quality improvement project has worked, helping others to understand what you did (so that the same results can be achieved somewhere else) is an important but often neglected task. Thus, I wonder… how should information about quality improvement be shared and presented so that quality improvement interventions can be reproduced in new contexts?
- We can share information face-to-face at work . . .
- or in lectures and teaching sessions . . .
- or in academic journals . . .
- or even on Twitter!
In the first blog post of a short series I will get to grips with the basics:
What is quality improvement? And what is theory? I’ll need to know at least a little about both of these things, before I can think about how they might work together to make our healthcare system better.
- What is Quality Improvement?
‘Quality’ is a late 14th century word meaning ‘degree of goodness’. In the NHS, good quality care should include all three domains of quality – patient safety, clinical effectiveness, and patient experience. Quality improvement (QI) can involve enhancing any one of these aspects of quality. A longer definition explains that QI involves the “combined and unceasing efforts of everyone—healthcare professionals, patients and their families, researchers, payers, planners and educators—to make the changes that will lead to better patient outcomes (health), better system performance (care) and better professional development”.
QI often uses specific techniques such as Plan Do Study Act cycles and SPC (Statistical Process Control). Using structured methods helps in identifying problems, selecting and testing interventions, and measuring changes. The Health Foundation and NHS England have produced helpful guides on how to use such techniques well.
Some great examples of QI projects and interventions were showcased at the recent Health Education East Midlands Quality Improvement Forum. For example, Maheswaran and colleagues at Kettering General Hospital designed some stickers for weekend discharge plans to help doctors to identify quickly whether a patient is medically fit for discharge. More broadly, healthcare staff can intervene in many different ways to improve care.
- Health Education East Midlands Quality Improvement Forum 2015 Programme
- Poster by Maheswaran and colleagues from the Quality Improvement forum
- What is theory?
A theory is a set of interrelated ideas and can provide a foundation for understanding something. Scholars love theories, but clinicians use them too, probably more often than we think during our everyday work.
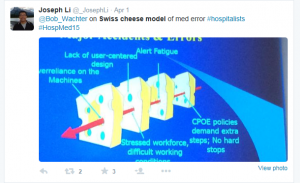
One example that fits this definition is the Swiss cheese model of patient safety, originally proposed by James Reason. There is debate over its status as a theory of accident causation as it functions like a ‘model’, and recent criticism has highlighted the limitations to its usefulness. Despite these problems, the image of ‘Swiss cheese’ as a process of identifying error is still recognisable by a large proportion of clinical staff. We tweet Swiss cheese images……. A lot!:
And our professional bodies (such as the Royal College of Nursing) encourage us to recognise the Swiss cheese model so that we can understand how to make our patients safer.
Personally, I associate the Swiss cheese model with meetings we hold at the hospital when we needed to address a complaint. In these situations the model was used to identify a trigger for the error – such as chaotic working environments, stress, too little staff, or frequent staff changes – because this is what starts the cascade towards an accident. We then try to recognise the things that errors hate – safe communication, clear agreements, and calmness even in emergencies. By reflecting on what happened and by working through the holes in the cheese we can then come up with a solution to make sure the accident does not happen again.
Another example of everyday use of theory is in behaviour change, which has been used in the routine management of low back pain, and is recommended by the National Institute for Health and Clinical Excellence (NICE) guidance. This means using practical techniques such as signed exercise agreements, verbalising goals, or providing written educational material in order to alter patients’ day-to-day habits and thus reduce their pain. These techniques have all grown out of the scholarly work on behaviour change theory, and they have been critical to maintaining good patient care throughout my 14 years in practice as a physiotherapist.
Until recently I hadn’t thought about how much I already use theory in my clinical work. In my next blog I’m going to think about theory I’m not already using, and how it might help me in my ability to carry out quality improvement work. Watch this space!







 Subscribe to Emma Jones's posts
Subscribe to Emma Jones's posts
Personally I think the definition of quality is multi-dimensional and subjective, thus the reason that the NHS struggles to ensure quality care is delivered everytime. Practioners will no doubt have a different perception of quality than patients; practitioners might consider quality to be the efficiency and the standard of care they provide whereas a patient may describe quality as timely care. In essence quality is anything anyone wants it to be. This combined with the numerous available measures of quality make quality improvement challenging.
And all of this leaves us quality improvment researchers with the bigger challenge of finding a useful theory to help explain how quality improvement happens in practice. 🙂
Looking forward to your next installment.
Barbara O’Donnell PhD student UWS
I agree that QI can means many things to many people but feel strongly that any project needs sound stakeholder involvement. Being able to measure improvement means being flexible to the changing dynamics between patients and staff and this can often lead to inconsistent methodology. That’s real life and what happens in reality!! Still powerful stuff even if reproducibility is limited.
Thanks both for these comments, as a novice blogger (and one who is reasonably challenged by smart phones and all things ‘Information Technology’ related) I am really enjoying being able to engage in discussion with you through this web-based mechanism! I am pleased that this blog has struck a chord and I agree with you both – quality is difficult to define and I also find it to be an emotive concept which means different things to different people. It is a joy to me that I can continue to discover more about what QI means and why it is important through continuing to care for patients, and I too would like to see more growth in opportunities for patients to become more involved in the design, delivery and reporting of QI projects. I will watch the field with interest to see how this evolves!